Is Overpronation a Problem?
When I was taught as a student I was led to believe and believed over pronation was the route of all evil. Is that true? Well in short it’s not. I find using a picture rather than words is better when describing an over pronated foot.
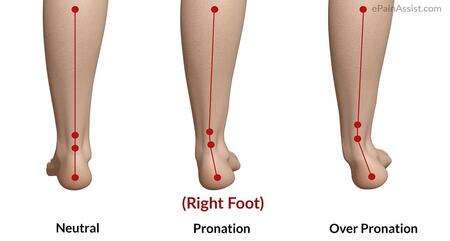
What are the symptoms often associated with pronation?
These include: Plantarfascitis which is often referred to as pain in the sole of the foot, posterior tibialis tendonopathy which is pain that you might experience that runs from the inside of the ankle down into the arch of the foot and knee pain are commonly referred to as causes of over pronation “the list goes on.”
If you look at the literature there is not much robust evidence to support this so clinicians need to be very careful when diagnosing the cause of a lower limb complaint from a client and look at the bigger picture.
When does it become a problem?
A couple of recent meta-analysis (a meta-analysis reviews all related studies using a specific criteria to determine what the collective results mean) found that pronation is a risk factor for injury and although a small one, it’s a significant one that must be given close consideration (Jasper et al and Bradley et al).
What causes pronation?
So if we know pronation can be problematic we need to know what causes it. There are a few things we know for sure that result in pronation and these include:
- tight calf muscle will cause the mid- foot to collapse which results in pronation
- the relationship of the rear foot and fore foot can cause the foot to pronate
- weak muscles that externally rotate the hip or invert the foot can cause the foot to pronate
So these are some of the things a clinician will be able to identify during assessment and be able to prescribe a treatment plan for.
What tools assess pronation?
Pronation can be caused by a range of things and can be seen in different planes of the foot. The foot posture index is a very useful tool that we use in Podiatry Shetland as it allows the podiatrist to look at the foot in different planes. Things we might see are a bulging mid-foot, a collapsed arch or the position of the heel turning in the way.
The podiatrist might also want to asses muscle strength (external rotators of the hip) and resistance when inverting the foot. Gait Analysis is also very important to assess the lower limb in function.
All of this together should enable the podiatrist to consider the right treatment plan.
What are the treatment options?
With regard to treatment it depends what the cause is. If it’s tight or weak muscles that must be addressed through the appropriate physical therapy, but that may also be complemented by an orthotic, strapping or even a specific feature in the running shoe.
If you would like to know more about the features you should expect to see in a Motion-Control running shoe look out our advice publications.
To get further updates and tips from Podiatry Shetland why not follow us on Facebook, Pinterest, Twitter and Instagram
